How the goal of weight loss can undermine health—considerations and resources for health practitioners
Weight is undeniably correlated to an increased risk of many health conditions, such as diabetes, cardiovascular disease and cancer.
However, is the pursuit of weight loss the answer to reducing these health risks or managing such health conditions once present?
In a webinar with the Global Weight Management Federation, I addressed this question.
Now, if you know anything about my approach to health and nutrition, having read any of my previous blogs or my book, Joyful Eating, you’ll know what my answer is. However, to prepare myself for questions and potential objections I may receive from those who subscribe to and support weight management in their professional practice, I compiled a list of useful resources, which you can find below the summary of the key points I covered in the webinar.
The fundamental reason the goal of weight loss can undermine health
In the book Joyful Eating, I explore the many reasons why the goal of weight loss can backfire in improving someone’s health. I discuss the negative psychological and physiological impacts of yo-yo dieting and weight cycling, how the stress associated with dieting can disrupt digestion and slow metabolism, and how diets promote disordered eating. Quite simply, I present the evidence that diets don’t work.
However, the fundamental reason why the goal of weight loss undermines efforts for improved health, and on which diet mentality stems, is weight bias and weight stigma.
I acknowledge that this may seem counterintuitive. We’ve been led to believe that telling someone they need to lose weight—eat less, exercise more—is a motivational cheer. However, the research shows that the opposite is true; rather than motivating, the shame of weight stigma is not only demotivating but also harmful to a person’s health.
Weight stigma is harmful to health
Studies show that weight stigma can:
- result in eating more and feeling more out of control with eating;
- cause avoidance of exercise;
- reduce self-efficacy (individual’s belief in their capacity to execute behaviours to attain their goals);
- increase stress;
- raise cortisol (an obesogenic hormone);
- lead to poor metabolic health;
- increase inflammation and metabolic syndrome;
- increase rates of anxiety, depression and mental health issues;
- result in care avoidance, misidentification or delay in diagnosis;
- increase risk of dying, independent of BMI (body mass index); and
- ironically increase weight gain (see Tomiyama, 2018 for a thorough summary of the evidence on how weight stigma harms health).
Furthermore, weight stigma has health implications in its own right. One study demonstrated that the perception of oneself as being overweight, no matter of BMI, is associated with biological markers of poorer health, including increased depressive symptoms, and physiological dysregulation of cardiovascular, inflammatory and metabolic functioning (Daly, 2017).
Given the psychological and physiological impacts of weight stigma, we can’t untangle weight stigma from weight as a health risk.
If we ditch the goal of weight loss, then what?
Given that weight stigma does more to harm than promote health, it’s time that we stopped recommending weight loss. If our aim truly is to help people improve their health, we need to put our efforts and emphasis on lifestyle behaviours that have proven health-promoting benefits, not on weight.
A study of 11,000 adults in the United States examined the association between healthy lifestyle habits—eating 5 or more fruits and vegetables a day, exercising regularly, consuming alcohol in moderation and not smoking—and mortality across BMI. They found that adopting these healthy lifestyle habits decreased mortality across all BMI categories. When all four healthy lifestyle habits were adopted there was no difference in mortality between the BMI of ‘normal weight’, ‘overweight’ and ‘obese’ (Matheson, 2012).
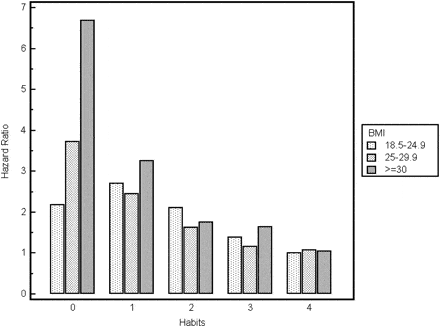
Figure 1. Hazard ratio for all-cause mortality by body mass index (kg/m2) and number of healthy habits (i.e. fruit and vegetable intake, tobacco, exercise, alcohol). Sourced from: Matheson, 2012.
In further support of this is the ever-increasing research on the Health at Every Size® (HAES) approach, which has demonstrated that people can improve their health at any size. A review by Bacon and Aphramor evaluated the evidence. They found that ‘randomized controlled clinical trials indicate that a HAES approach is associated with statistically and clinically relevant improvements in physiological measures (e.g., blood pressure, blood lipids), health behaviours (e.g., eating and activity habits, dietary quality), and psychosocial outcomes (such as self-esteem and body image), and that HAES achieves these health outcomes more successfully than weight loss treatment and without the contraindications associated with a weight focus.’ I highly recommend this paper if you’d like to explore the scientific rationale for shifting from a weight-focused approach to a HAES approach.
Not weight loss by another guise
Please don’t misinterpret the above to mean that if we put weight to the side and focus on health, a person’s weight will adjust to what is healthy for them. This thinking continues to imply that there is a healthy weight that a person will or should attain. What I’m saying is that we should no longer consider weight at all.
The research is clear—focusing on weight loss does not lead to improved health but does more to perpetuate weight stigma. There is no need to focus on weight for people to adopt lifestyle behaviours that promote psychological and physiological health.
How, as health practitioners, can we focus on improved health without the goal of weight loss?

You can support your clients to create healthy lifestyle habits they can enjoy and sustain long-term to improve well-being, irrespective of weight loss.
The first step is to shift the focus away from weight to behaviours that promote health while rejecting weight bias. Weight bias is the preference of people in smaller bodies, which often comes with an assumption that they are healthier than people in larger bodies. Weight stigma is the negative impact of weight bias.
Since weight bias is rife in society and among health professionals, our role should include reducing the burden of weight stigma.
Weight-inclusive practice
If you want to provide a weight-inclusive practice where your focus is on health rather than weight, you’ll find ample ideas in the below resources.
First, to consider is how your practice may perpetuate weight bias and weight stigma, explicitly or implicitly. Weight bias may be present in marketing imagery and wording, intake forms, office setup, and how you talk to your clients about weight or weight loss. Some examples of weight bias and stigmatisation may be:
- Before and after images suggest that one body is better than another and that health and happiness can be determined by a photo—which it cannot!
- Images of people being active or eating healthily who are only in smaller bodies is implicit weight bias. People need to see their own bodies, or a variety of body shapes, sizes, ethnicities and genders, represented and partaking in health-promoting behaviours and looking happy and vibrant.
- Complementary weightism and appearance-related compliments such as telling a client, ‘you’ve lost weight, good on you’, ‘you’re looking great’, ‘let’s blast that cellulite’ are stigmatising as it reinforces that their body is either good or bad based on their weight.
- Congratulating or celebrating weight loss reinforces that a lower weight is better than a higher weight and thus perpetuates weight stigma. Any program, whether diet or lifestyle program, that celebrates weight loss is weight biased. If you’re wondering what to say instead of congratulating or saying, ‘That’s great’ when a client tells you they’ve lost weight, think about what you’d say to someone of a normal weight who tells you about a lifestyle change they’ve made or an accomplishment (e.g. ran their first 5km). You can employ motivational interviewing and positive psychology techniques to help clients improve their health without a focus on weight or appearance. You could ask them how the changes have made them feel, whether they could sustain them long-term, whether they’d like to try something else or would like to build on the healthy lifestyle behaviours they’ve adopted. Furthermore, you may want to begin the conversation by reinforcing that you practice weight neutrality and thus do not focus on weight loss but instead encourage them to think about what makes them feel better in their everyday lives, physically, mentally and emotionally.
- Prescribing to a person in a larger body what would be considered disordered eating or unhealthy behaviour in someone of an ‘underweight’ or ‘normal’ BMI, such as unrealistic restriction, skipping meals, appetite suppressants, exercising on an empty stomach, laxative teas, fasting etc.
- Weighing clients at all, but especially if they’re seeing you for a completely unrelated health condition, say an ingrown toenail or they want to improve their fitness. The automatic weighing of people can lead them to avoid care or taking up health-promoting behaviours, such as attending personal training sessions or seeing a nutritionist. Avoidance of care may be due to a fear of judgement or receiving unsolicited advice about weight loss. If you weigh your clients, consider why—what benefit does it provide or does it do more to perpetuate shame?
If you advise or help people in larger bodies lose weight (or congratulate them when they do), you are perpetuating weight bias.
It is possible, however, to guide and support your clients to adopt lifestyle behaviours for improved health, should this be a priority for them (it may not always be), without any consideration of weight.
Shedding our own weight bias and avoiding perpetuating the weight stigma that our clients feel is likely to take time and require in-depth exploration of our own beliefs and the way we practice. However, it is possible. There are now many nutritionists, dietitians, health coaches, personal trainers and counsellors who are supporting their clients through the weight-neutral approaches of non-diet practice, weight-inclusiveness, Health at Every Size®, intuitive and mindful eating. I hope you join us.
Want to learn more about the impacts of weight stigma, taking a non-diet and weight-neutral approach, Health at Every Size®, and how to support your clients without an emphasis on weight?
Further Reading – Associated Blogs on Joyful Eating
- How the goal of weight loss can sabotage your health
- 4 reasons why you shouldn’t adopt mindful eating for weight loss
Resources and Further Information
- Joyful Eating Companion Workbook, a free PDF download, contains activities that can be used with coaching clients for them to explore their relationship with food and their body.
- HAES® (Health at Every Size).
- HAES® Australia.
- Association for Size Diversity and Health (ASDAH). Download the HAES® Principles.
- Unpacking Weight Science Podcast, with Fiona Willer, Advanced Accredited Practising Dietitian.
- Learn about Intuitive Eating and the 10 Principles of Intuitive Eating.
- Health, Not Diets: Training and workshops in the Non-Diet Approach.
- The free eBook, Everything You’ve Been Told About Weight Loss is Bull Shit by Clinical Psychologist, Louise Adams and Advanced Accredited Practising Dietitian, Fiona Willer, provides a great summary of why diets don’t work by busting the ten top myths of dieting. It is chocked full of scientific evidence if you want to read on the topic further.
Short Courses and Study
- Free Open Learning Course by Fiona Willer: Introduction to the Non-Diet Approach covers weight bias, what the weight-neutral and non-diet approaches are and the HAES principles.
- A$79 Open Learning Course by Fiona Willer: Unpacking Weight Science.
Recommended Podcasts
- Food Psych Podcast with Christy Harrison MPH, RD, CDN is a podcast about intuitive eating, Health at Every Size® and body liberation.
- The Mindful Dietitian Podcast hosted by Fiona Sutherland, Accredited Practising Dietitian, Non-Diet Dietitian, Body-Inclusive Health Practitioner & Yoga Teacher covers topics of body inclusivity, Health at Every Size®, non-diet approach and mindfulness-based practice.
- All Fired Up! Podcast is hosted by clinical psychologist Louise Adams and focused on delving into diet culture and fighting for equality, justice and freedom
Further Reading – Books
- My own book. Tansy Boggon.Joyful Eating: How to Break Free of Diets and Make Peace with Your Body. Lulu Publishing; 2019.
- Evelyn Tribole and Elyse Resch. Intuitive Eating: A Revolutionary Program that Works. St. Martin’s Griffin, New York; 2012. Now in its fourth edition, published as, Intuitive Eating: An Anti-Diet Revolutionary Approach.
- Linda Bacon. Health at Every Size: The Surprising Truth About Your Weight. Dallas: TX BenBella Books; 2010.
- Fiona Willer. The Non-Diet Approach Guidebook for Dietitians: A How-To Guide for Applying the Non-Diet Approach to Individual Dietetic Counselling. NutritionSense Allied Health; 2013.
Further Reading – Key Scientific Papers
- Bacon L., Aphramor L. Weight science: evaluating the evidence for a paradigm shift. Nutr J; 2011. 10: 9.
- Tylka, T.L., Annunziato R., Burgard, D., Danielsdottir, S., Shuman, E., Davis, C., Calogero, R.M. The weight-inclusive versus weight-normative approach to health: Evaluating the evidence for prioritizing well-being over weight loss. Journal of Obesity; 2014.
- Tomiyama J.A., Carr D., Granberg E.M., Major B, Robinson E., Sutin A.R., Brewis A. How and why weight stigma drives the obesity ‘epidemic’ and harms health. BMC Med. 2018; 16: 123.
- Matheson E.M., King D.E., Everett C.J. Healthy lifestyle habits and mortality in overweight and obese individuals. J Am Board Fam Med. 2012 Jan-Feb; 25(1): 9-15. Compared association of healthy lifestyle habits on mortality across BMI ranges, finding that healthy lifestyle habits are associated with a significant decreased in mortality regardless of baseline body mass index.
- Mann T., Tomiyama A.J., Westling E., Lew A.M., Samuels B., Chatman J. Medicare’s search for effective obesity treatments: diets are not the answer. Am Psychol. 2007 Apr; 62(3) :220-33. Key study that shows that one third to two-thirds of dieters regain more weight than they lost on their diets.
- Daly M., Robinson E., Sutin A.R. Does Knowing Hurt? Perceiving Oneself as Overweight Predicts Future Physical Health and Well-Being. Psychol Sci. 2017 Jul; 28(7): 872-881.


2 comments
Hello! I like your writing so much!
I need an expert in this area, maybe that is you!
I’m pleased you’ve found this blog useful. I look forward to sharing more with you.